If you’re a runner in Prosper, Frisco, or anywhere along the North Texas trails, you’ve probably either had plantar fasciitis or know someone who has. That first step out of bed in the morning — the one that feels like stepping on a nail — is unmistakable. So is the tightness that creeps in during the last mile of a long run, the heel pain that gets worse the more miles you log, and the sinking feeling that you’re going to have to stop running just when training was getting good.
Here’s the part most runners don’t hear: plantar fasciitis isn’t usually a foot problem. It’s the place where the symptom shows up, but the cause is almost always upstream — in your hips, your gait, your stride mechanics, or how your nervous system is coordinating the whole chain. Treat the foot in isolation and the pain comes back. Address what’s actually driving it, and most runners get back to training faster than they expect.
Here’s what’s really going on, and how to train through it without losing your fitness.
What Plantar Fasciitis Actually Is
The plantar fascia is a thick, fibrous band of tissue that runs from your heel bone to the base of your toes. It acts like a bowstring along the bottom of your foot — storing and releasing energy with every step you take. When you run, that tissue absorbs and redirects an enormous amount of force, repeatedly, for thousands of strides.
Plantar fasciitis is what happens when that tissue gets overloaded and starts to break down at the cellular level. Despite the “-itis” in the name, current research shows it’s not primarily an inflammation problem — it’s a degenerative one. The tissue is failing to repair itself faster than running is breaking it down. That’s why anti-inflammatories rarely fix it long-term, and why simply resting often doesn’t either: rest pauses the breakdown, but it doesn’t stimulate the tissue to actually rebuild.
Why Runners Get It More Than Anyone Else
Runners stack risk factors that few other populations face. A few of the big ones we see at our Prosper office:
Cumulative load. Running puts roughly 2–3 times your body weight through each foot, thousands of times per run. Even good tissue has a fatigue limit, and most plantar fasciitis cases show up during a training increase — new mileage, new pace, new terrain, a marathon block, a return from injury.
Hip and glute weakness. When your glutes don’t fire properly, your stride collapses inward. The arch of your foot has to compensate, the plantar fascia takes load it was never designed for, and the heel insertion gets hammered. This is one of the most common patterns we see — and it’s often invisible until pain shows up at the foot.
Calf and Achilles tightness. The plantar fascia is functionally continuous with the calf and Achilles. When the calf is tight or restricted, every step pulls extra tension through the heel and into the fascia. Calves get tight from running, sitting at a desk all day, sleeping in plantarflexion — a lot of things modern life does to us.
Gait and footstrike issues. Overstriding, heavy heel-strike, or a stride pattern that crosses the midline puts unusual load on the medial arch and heel. These patterns rarely correct themselves, and inserts don’t fix them.
Spinal and nervous system dysfunction. This one surprises a lot of runners. The nerves controlling your foot mechanics, glute activation, and lower-leg coordination all originate in your lumbar spine. When the nervous system isn’t communicating cleanly with the lower body, muscles fire late, compensation patterns build, and stress concentrates exactly where it shouldn’t.
What Doesn’t Work (or Only Half-Works)
Most runners try the same things, in the same order, before they finally get real help. Here’s the honest scorecard:
Shoe inserts and orthotics. Sometimes helpful, often not. Inserts support the arch passively, but they don’t fix the upstream mechanics that overloaded the fascia in the first place. Many runners feel a little better with them, then realize the pain just plateaus.
Rest. Time off helps the acute symptoms calm down, but as soon as you return to mileage, the pain often comes back. Rest without addressing the cause is a pause button, not a fix.
Anti-inflammatories. Reduce the pain signal, do nothing for the underlying tissue. Long-term use also has real downsides for athletes (gut, kidney, recovery).
Stretching alone. Calf and plantar fascia stretches help — but on their own they rarely resolve the problem in runners with persistent symptoms. They’re a piece of the puzzle, not the whole thing.
Corticosteroid injections. They can provide short-term relief, but research shows they don’t outperform non-invasive options at the 3- and 6-month marks, and repeated injections can actually weaken the plantar fascia and increase rupture risk — not a tradeoff most runners want.
What Actually Works (and Why)
The most effective plan addresses the foot, the upstream chain, and the tissue itself at the same time. Here’s what that looks like in practice.
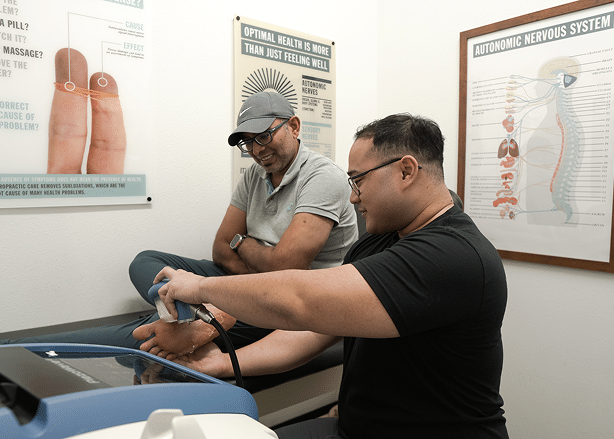
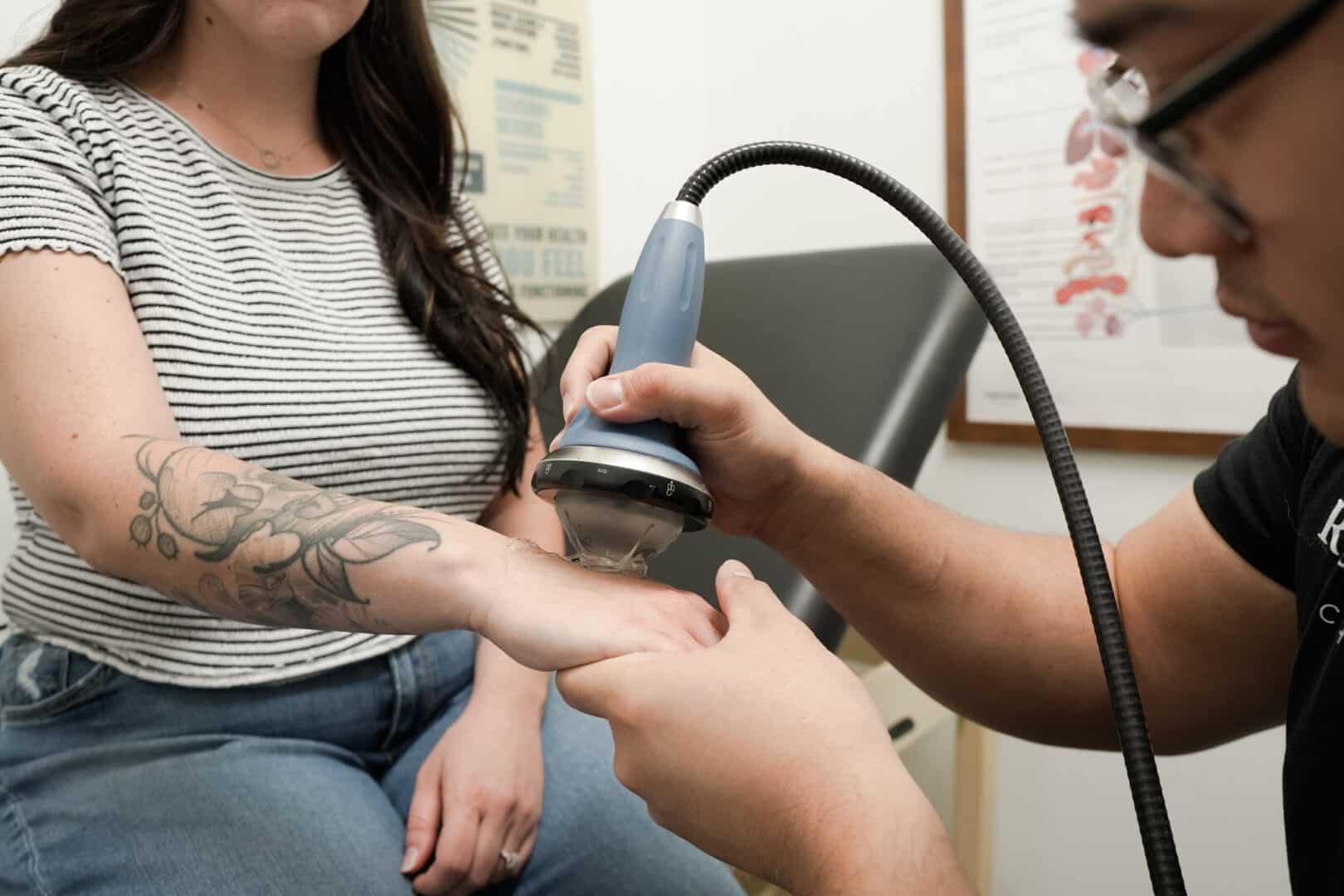
Shockwave Therapy
Shockwave therapy is one of the best-evidenced treatments for chronic plantar fasciitis — and one of the reasons it’s become standard care for runners who don’t want surgery or injections. Multiple 2024 meta-analyses comparing shockwave to other options found it as effective as corticosteroid injections for pain reduction, without the tissue-damage risk that comes with repeated steroid use.
What it actually does: focused acoustic pulses stimulate the plantar fascia to remodel and regenerate, increasing blood flow to a notoriously poorly-vascularized tissue and breaking up adhesions that have built up over months of dysfunction. For runners, that’s the missing piece — it doesn’t just calm symptoms, it stimulates the tissue to actually heal.
Most patients we see for plantar fasciitis need 3–6 sessions, spaced about a week or two apart. Sessions are short, you can usually keep running between them (with guidance), and most runners notice meaningful change within the first 2–3 visits. Learn more about how shockwave therapy works at Restoration →
Chiropractic Care for the Whole Chain
Because plantar fasciitis is almost always an upstream problem, addressing only the foot is incomplete. We use gentle, instrument-based adjustments (Torque Release Technique) combined with NASA-certified nervous system scanning to identify exactly where the chain is breaking down — the lumbar spine, the SI joints, the hips, the ankle — and correct it. When the nervous system communicates cleanly with the lower body again, glutes fire on time, stride mechanics clean up, and the fascia stops getting loaded the wrong way every single step.
Targeted Strength and Mobility Work
Once the mechanics are improving, the work shifts to making the changes stick. That usually means glute activation, hip stability, calf and Achilles mobility, and progressive loading of the plantar fascia itself (heavy slow calf raises off a step are a runner’s best friend here). We’ll walk you through a specific home program based on what your scan and exam show.
How to Keep Training While You Heal
This is the question every runner asks, and the answer is: in most cases, yes — with smart modifications. A few principles we coach runners through:
- Cut volume before you cut pace. Most plantar fasciitis is a volume problem, not an intensity problem. Drop your weekly mileage by 30–50% temporarily; keep the quality runs that don’t aggravate symptoms.
- Trade some miles for cross-training. Cycling and pool running maintain fitness without the repeated impact load. Two or three sessions a week can hold your aerobic base while the fascia recovers.
- Watch the morning pain. The first-step-out-of-bed test is your daily readiness check. Steady improvement week over week means the plan is working. Plateau or regression means something needs to change.
- Don’t train through sharp pain. Dull tightness that warms up in the first mile is usually fine. Sharp, localized pain that gets worse as you run is not. Listen to it.
- Rebuild gradually. When symptoms are settling, increase mileage by no more than 10% per week. Most plantar fasciitis flare-ups happen when runners go from feeling better to long-run-on-Saturday in the same week.
When to Get Evaluated
If your plantar fasciitis has been hanging on for more than a few weeks, isn’t responding to stretching and rest, or keeps coming back every time you ramp up training, it’s worth getting evaluated. Plantar fasciitis caught early is usually a quick fix. The chronic, six-months-and-counting version takes longer to resolve and can lead to compensation injuries elsewhere — calf strains, Achilles tendinopathy, knee pain, even hip and lower-back issues from the way you’ve been favoring the foot.
At Restoration Chiropractic in Prosper, every new patient starts with a full neurological scan, on-site digital X-rays where appropriate, and a doctor’s report walking you through exactly what we found and what the plan looks like. If your case is one shockwave and chiropractic care can resolve, we’ll tell you and we’ll show you the timeline. If it’s one that needs another specialist, we’ll tell you that too.
You don’t have to stop running. You just have to address what’s actually driving the pain.