If you’ve been told you have a herniated disc, you’re probably weighing your options — and surgery may already be on the table. Before you commit to a procedure, it’s worth understanding what the research actually says about non-surgical care, when surgery is genuinely warranted, and what most patients in your situation actually do.
Short version: most herniated discs heal without surgery. Conservative care — chiropractic, physical therapy, time, movement — resolves the majority of cases. Surgery is a real and necessary option for a smaller subset of patients, but it’s rarely the first step, and it’s rarely the only path forward.
Here’s how to think it through.
What Most People Don’t Know About Herniated Discs
Herniated discs are far more common than the panic around them suggests. MRI studies have repeatedly found that a significant percentage of asymptomatic adults — people with no back pain at all — have visible disc herniations on imaging. In other words, the herniation showing up on your MRI may or may not be the actual cause of your symptoms.
The body is also remarkably good at healing disc injuries on its own. Research has documented that more than half of disc herniations spontaneously reduce or fully resorb within months, even without active treatment. Larger, more dramatic herniations on imaging often resorb more readily than smaller ones — the opposite of what most patients assume.
This matters because it reframes the decision. A herniated disc isn’t typically a "fix it now or live with it" problem. It’s usually a "support the body’s natural healing process" problem.
The Standard Treatment Hierarchy
Most major orthopedic and neurosurgical guidelines recommend a stepped approach to herniated disc care, escalating only if conservative measures fail:
Step 1 — Conservative care (4–12 weeks). Activity modification, chiropractic care, physical therapy, anti-inflammatories, and gentle movement. The vast majority of patients improve significantly during this window.
Step 2 — Targeted intervention (if needed). Epidural steroid injections to reduce inflammation around the affected nerve. These provide temporary relief but don’t address the underlying issue.
Step 3 — Surgical consultation. Reserved for patients whose symptoms haven’t responded to 6–12 weeks of conservative care, or who have specific red-flag symptoms (more on those below).
Skipping straight to step 3 isn’t how most reputable specialists practice. If you’ve been told surgery is your only option without first attempting conservative care, a second opinion is reasonable.
How the Options Actually Compare
Chiropractic Care
What it does: Restores spinal alignment and motion, reduces pressure on the affected disc and nerves, addresses compensation patterns that develop around the injury.
Best for: Most non-emergency herniated disc cases, especially those involving back pain, sciatica, or radiating leg pain without progressive neurological deficits.
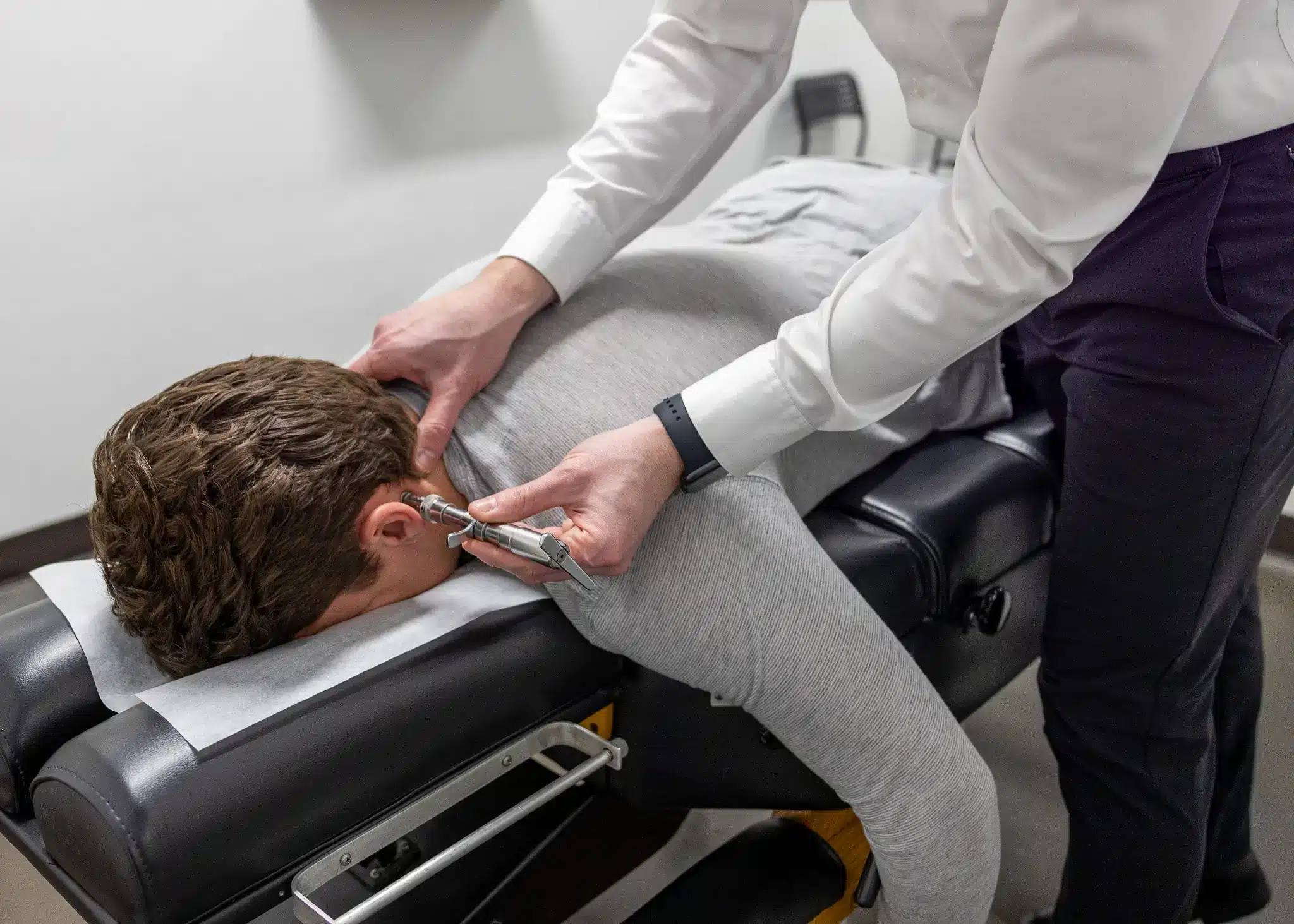
Tradeoffs: Requires a series of visits over weeks, not a single fix. Technique matters significantly — high-velocity manual adjustments aren’t appropriate for every disc patient, which is why we use the gentler, instrument-based Torque Release Technique.
Physical Therapy
What it does: Strengthens the muscles supporting the spine, improves posture and body mechanics, teaches movement patterns that reduce future injury risk.
Best for: Patients who need to rebuild strength and stability, often used alongside chiropractic care for compounding benefit.
Tradeoffs: Doesn’t directly address spinal alignment or nerve interference; works best when paired with care that does.
Epidural Steroid Injections
What it does: Delivers anti-inflammatory medication directly to the area around the affected nerve to reduce pain and swelling.
Best for: Patients with severe inflammatory pain who need short-term relief, often as a bridge to other treatments.
Tradeoffs: Provides temporary symptom relief without addressing the underlying disc or alignment issue. Effects typically last weeks to a few months. Repeated injections carry diminishing returns and potential side effects.
Surgery (Microdiscectomy or Laminectomy)
What it does: Surgically removes the portion of the disc pressing on the affected nerve.
Best for: Patients with severe, progressive neurological symptoms (significant muscle weakness, loss of bladder/bowel control), or those whose pain has not responded to several months of conservative care.
Tradeoffs: Surgical procedure with associated recovery time and risks. Outcomes are generally good for properly selected candidates, but long-term studies show that conservative care often produces comparable outcomes for non-emergency cases when given enough time.
When You Genuinely Should Consider Surgery
We’re honest with our patients: surgery is the right answer for some herniated disc cases. If any of the following apply to you, you should seek immediate medical evaluation rather than starting with conservative care:
- Loss of bladder or bowel control, or numbness in the groin or saddle area — these are signs of cauda equina syndrome and require emergency surgical evaluation
- Progressive muscle weakness — for example, foot drop, or weakness that’s clearly getting worse over days or weeks
- Severe, intractable pain that doesn’t respond to any conservative measures over a meaningful period
- Pain and dysfunction that has persisted for several months despite a real, committed effort at conservative care
If none of these apply to you, conservative care is almost always worth trying first.
What the Research Shows
The research on chiropractic care for herniated discs has grown substantially over the past two decades and is broadly favorable.
Studies tracking patients with confirmed disc herniations have found that a significant majority report meaningful improvement with spinal adjustments — often within weeks. MRI follow-up studies have documented reductions in herniation size and nerve compression after courses of chiropractic care, sometimes substantial.
Comparative studies on chiropractic versus surgery for non-emergency disc herniation are particularly interesting: at one and two years out, patients who started with conservative care often report outcomes similar to those who had surgery, with the obvious advantage of avoiding a procedure entirely.
A 2014 study published in the Journal of Manipulative and Physiological Therapeutics followed patients with MRI-confirmed lumbar disc herniation receiving chiropractic care. Roughly 60% reported clinically meaningful improvement after just two weeks, and the majority maintained those gains at three months and one year.
None of this means chiropractic is the right answer for every patient or every case. It does mean that the data supports trying it before assuming surgery is necessary.
How to Decide What’s Right for You
The honest answer is that the decision depends on your specific situation — the severity of your symptoms, how long they’ve been going on, what you’ve already tried, and what your imaging actually shows.
A good first step is a thorough evaluation. At Restoration Chiropractic, every new patient starts with a full neurological scan, on-site digital X-rays, and a doctor’s report walking through exactly what we found and what your options look like. If your case is one that genuinely warrants surgical evaluation, we’ll tell you. If it’s one we can help with, we’ll lay out a realistic plan with a realistic timeline.
For most herniated disc patients, the path forward isn’t a coin flip between "live with it" and "go under the knife." There’s a middle road, and the research and outcomes support starting there.